Why Are The Veins In My Legs So Dark?
So you’ve noticed dark bluish veins appear in your legs. Maybe you’ve had then for some time and never thought more of them until now – or maybe they’ve recently become noticeable. With the well-known link between our veins and our circulation, changes to the appearance of our veins can be distressing. Today, we’re setting the record straight about the appearance of dark veins in the legs, why they occur, and when these veins can be a warning sign of something worse.
Veins: What do they do?
First thing’s first: we have veins all around our body, whether we can see them or not. They play a very important role – helping return the blood that has been pushed out from our heart and to every corner of our bodies by our arteries back to the heart.
As we all know, working against gravity is no easy feat. Veins are able to carry blood against gravity up to the heart through a series of one-way valves that prevent the blood from going backwards, combined with muscles surrounding the vessels which contract and help pump blood to the heart.
Visible veins appear when there are problems returning the blood back to the heart
As with any vessel or tissue, healthy vein function can be impaired and compromised. Problems with the vein valves, the surrounding muscles or blood itself can result in blood pooling inside the vein. This means that pressure builds and the vessel walls weaken, causing the vein to bulge and twist and produce a noticeable spider vein or varicose vein.
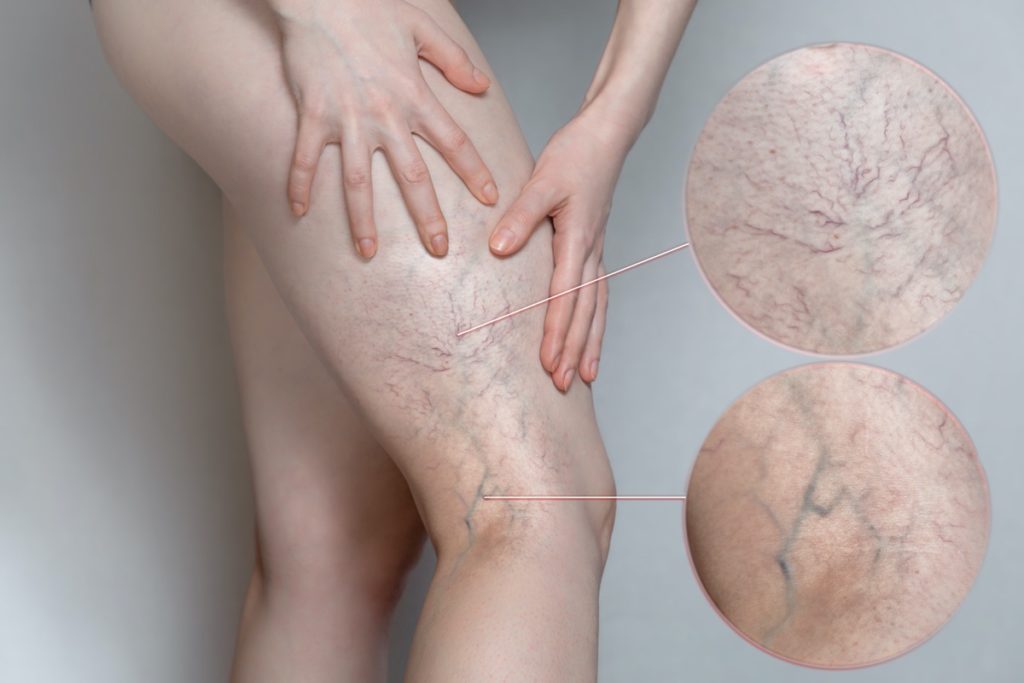
- Spider vein – a very small and prominent blood vessel that often takes the form of a spider web pattern – having a central point and then branching out. These veins may be red, purple, or blue. They’ll most often appear on the legs or the face
- Varicose vein – much bigger than spider veins, varicose veins are the most common type of vein abnormality – and often the cause of prominent blue veins in the legs. They tend to bulge out from the skin, giving them a worm-like appearance. They can develop anywhere on the body but most often arise in the feet and ankles
If these vein changes have affected you, know that you are not alone. Up to 60% of adults will experience changes in the appearance of their veins. Alongside noticing the appearance of the veins, you may feel:
- Foot & leg aches and cramps
- Throbbing, burning and tingling
- Tired, heavy legs
- Foot & leg swelling
- Inflammation & itchiness
Are spider veins and varicose veins dangerous?
The good news is that while dark or prominent veins may be cosmetically unappealing, their presence alone does not mean that your health is immediately in danger. They can, however, indicate an increased risk of two important problems:
1. Blood clots. The blood that pools in large veins can in some circumstances clot. If the clots travel to other areas of the body, this can result in an embolism (a blockage in an important vessel).
2. Venous ulcers. When blood and other fluids buildup and pool, ulcers can form which may bleed and even become infected.
This is why it’s important to bring any concerns you have to your doctor at your next appointment – and let us know too!
Who is at risk of developing dark, prominent veins?
Women are twice as susceptible as men, though problems with the veins can affect anyone. This is largely due to hormonal changes throughout the various stages of a woman’s life. If your job keeps you on your feet, like if you’re a tradie or healthcare worker, you may also have an increased risk. Other risk factors include:
- Increasing age – as we age, our valves can wear down and they may be weaker and lose elasticity
- Increasing weight & obesity – extra weight on the body can put extra pressure on the veins
- A decrease in physical activity & movement
- Pregnancy – as a result of hormonal changes, combined with the increase in blood volume and pressure on the veins from the fetus, the woman is more vulnerable to developing varicose veins
- A history of injury
- Surgery
- A family history of venous insufficiency – if your parents had varicose veins, your chance of having them is significantly greater
- Standing for long periods at work – doesn’t allow your blood to flow as well as it should
Treating varicose veins
While it’s important to have your GP involved in your care and they may choose to refer you to a vein specialist, here at Marlborough Podiatry, we help you manage your symptoms using:
- Compression stockings
- Exercises targeted at promoting circulation in the feet and legs, especially at the calves
- Helping improve your mobility so you can walk or exercise daily
- Footwear to assist your mobility and help you feel comfortable on your feet
Every treatment plan is tailored to your unique needs by our experienced podiatry team. To get the best results, don’t forget to:
- Limit long periods of sitting or standing as much as possible
- Elevate your legs periodically, this can help with promoting blood return and reducing swelling
- Get your 30 minutes of exercise every day
- Limit high heel wear – flat shoes better work your calf muscles and help blood flow in this area
Book your appointment with us by calling 03 972 2927 or book online here.
